Rootcanals
What is Root Canal Therapy?
Unraveling the Misunderstood Dental Procedure
Introduction
Root canal therapy, often simply called a root canal, is a dental procedure that has garnered a reputation that can often be misleading. Far from the painful treatment it’s often thought to be, root canal therapy is actually a pain-relieving, tooth-saving procedure. This article aims to demystify root canal therapy, explaining what it is, why it’s necessary, and what the procedure entails.
Understanding Root Canal Therapy
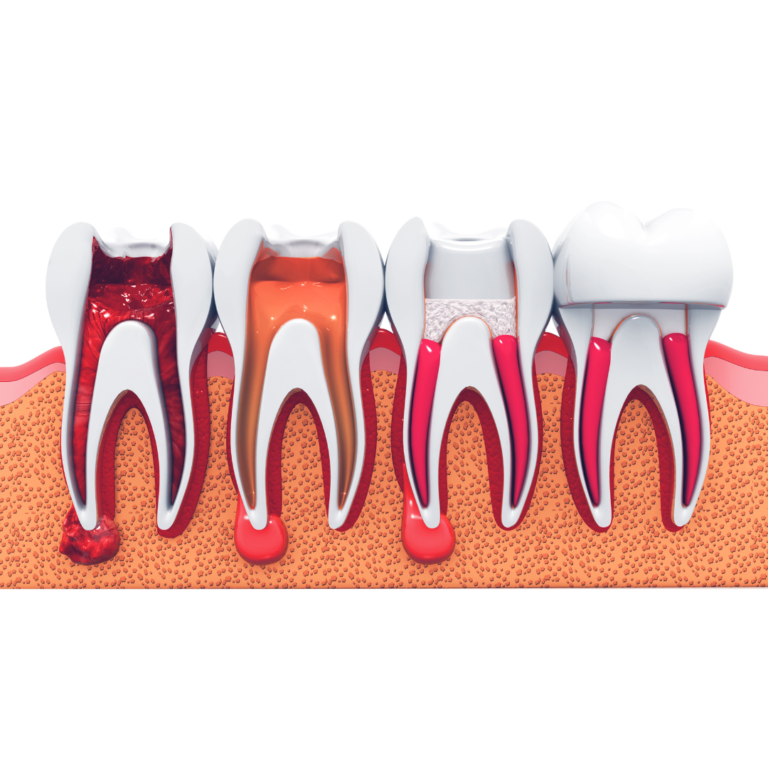
Root canal therapy is a treatment used to repair and save a tooth that is badly decayed or infected. The procedure involves removing the damaged area of the tooth (the pulp), cleaning and disinfecting it, and then filling and sealing it. The common causes affecting the pulp are a cracked tooth, a deep cavity, repeated dental treatment to the tooth, or trauma.
The Pulp: Heart of the Tooth
The tooth’s pulp is the soft area within the center of the tooth and extends down into the roots. The pulp contains nerves, blood vessels, and connective tissue and is responsible for the growth and development of the tooth during childhood. Once a tooth is fully mature, it can survive without the pulp because the surrounding tissues continue to nourish the tooth.
Mountain View Pointe Dental's Complete Guide To Root Canal Therapy
Why Root Canal Therapy Is Necessary: A Closer Look
Root canal therapy is often a necessary and crucial procedure in dental care, aimed at addressing problems within the innermost part of the tooth. Let’s delve deeper into the reasons why this treatment is essential.
Infection and Decay: The Core Issue
- Pulp Damage: Inside each tooth is a soft tissue known as the pulp, which contains nerves, blood vessels, and connective tissues. The pulp can become damaged due to deep decay, repeated dental procedures, cracks or chips in the tooth, or traumatic injury.
- Bacterial Infection: When the pulp is damaged, bacteria can enter and multiply within the pulp chamber. This bacterial growth can cause an infection or abscess, which is a pus-filled pocket that forms at the end of the tooth’s roots.
- Spread of Infection: Without treatment, the infection can spread beyond the tooth, potentially leading to swelling that may spread to other areas of the face, neck, or head. In severe cases, a bone loss around the tip of the root can occur.
Symptoms Indicating the Need for Root Canal Therapy
Understanding the symptoms that necessitate root canal therapy is crucial in seeking timely dental intervention.
- Severe Toothache: Pain is often the most noticeable symptom. A toothache that becomes more severe when biting down, chewing, or applying pressure is a telling sign. The pain might also persist or become more intense when lying down.
- Prolonged Sensitivity: Sensitivity to hot or cold temperatures that lingers long after the temperature stimulus is removed can indicate nerve damage or death, necessitating a root canal
- Discoloration of the Tooth: A tooth that becomes discolored (often turning grayish or blackish) can indicate that the nerve inside the tooth is dying or dead, leading to the buildup of waste products and staining the tooth from the inside.
- Swelling and Tenderness in the Gums: Swollen or tender gums around the affected tooth often accompany an infected tooth. This can sometimes manifest as a small, pimple-like bump on the gums, known as a dental abscess.
- No Symptoms: In some cases, a tooth may require root canal therapy without presenting any symptoms. This scenario can occur when the nerve inside the tooth has died but hasn’t yet become infected. Regular dental checkups can help identify these situations.
The Procedure of Root Canal Therapy: An In-Depth Explanation
Root canal therapy is a detailed and meticulous procedure designed to save a tooth that is severely decayed or infected. Let’s explore each step of this important dental treatment in greater detail:
1. Diagnosis and X-ray
- Initial Evaluation: The process begins with a comprehensive evaluation of the affected tooth. The dentist assesses symptoms and may probe the tooth to determine the extent of the issue.
- X-ray Imaging: X-rays are crucial for visualizing the tooth’s structure, particularly the root canals and surrounding bone. They help the dentist see the shape of the root canals and check for signs of infection in the bone around the tooth. This step is vital in planning the procedure and determining how to approach the treatment.
2. Anesthesia
- Local Anesthesia: To ensure patient comfort, local anesthesia is administered to the area surrounding the affected tooth. This step is crucial to make the procedure virtually painless.
- Numbing the Tooth: The anesthesia numbs the tooth and surrounding tissues, allowing the dentist to perform the procedure without causing pain. Patients might feel some pressure, but the process should not be painful.
3. Pulpectomy: Removing the Infected Pulp
- Accessing the Pulp: The dentist drills an opening in the crown of the tooth to access the pulp chamber.
- Removing Diseased Tissue: Using special instruments, the dentist carefully removes the infected or inflamed pulp from within the tooth’s canals. This step is known as a pulpectomy.
- Debridement: The dentist meticulously cleans out the canals to remove all traces of infected material, ensuring that the infection is thoroughly addressed.
4. Cleaning and Sealing the Tooth
- Cleaning the Canals: After the pulp has been removed, the canals are thoroughly cleaned and disinfected to remove any remaining bacteria and debris. This may involve a combination of manual and mechanical techniques, along with irrigating solutions.
- Shaping for Filling: The canals are then shaped and prepared to receive the filling material.
- Sealing the Tooth: Once cleaned, the interior of the tooth is filled and sealed with a rubber-like material called gutta-percha. This material helps to prevent bacteria from re-entering the tooth and causing further infection.
- Temporary Filling: In some cases, a temporary filling may be placed on the opening of the tooth to protect it between appointments.
5. Restoring the Tooth
- Final Restoration: Depending on the extent of the decay and the tooth’s structural integrity, the tooth will either be restored with a filling or, more commonly, with a crown. A crown provides added strength and protection, especially for teeth that have been significantly weakened.
- Crown Fitting: If a crown is needed, impressions of the tooth are taken, and a custom crown is created. Once ready, the crown is fitted and cemented onto the tooth, restoring its shape, appearance, and functionality.
Recovery and Aftercare Following Root Canal Therapy
After undergoing root canal therapy, proper recovery and aftercare are essential to ensure the success of the treatment and the longevity of the tooth. Here’s a detailed look at what you can expect during the recovery period and the best practices for aftercare.
Post-Procedure Care
- Initial Sensitivity: After the anesthesia wears off, it’s common to experience some sensitivity in the treated tooth. This sensitivity is typically due to natural tissue inflammation, especially if there was pain or infection prior to the procedure.
- Managing Discomfort: Over-the-counter pain relievers, such as ibuprofen or acetaminophen, can be effective in managing any discomfort. It’s important to follow the dosage instructions provided by your dentist or on the medication label.
- Minimizing Swelling: If there is swelling, a cold compress applied to the cheek area can help reduce it.
Oral Hygiene: Crucial for Healing
- Gentle Brushing: Continue to brush your teeth gently but thoroughly, being cautious around the treated area. Using a soft-bristled toothbrush can help minimize irritation.
- Flossing Carefully: Floss daily, but be gentle with the treated tooth. Avoid snapping the floss into the gums, which can cause discomfort or bleeding.
- Mouthwash: An antiseptic mouthwash can also be used to help keep the mouth clean, but it’s best to avoid using it immediately after the procedure as it might cause irritation. Consult your dentist on when to resume using mouthwash.
- Regular Check-ups: Follow-up appointments with your dentist are important to monitor the healing of the tooth and the success of the root canal treatment.
Diet Considerations: Protecting Your Tooth
- Soft Foods: Stick to soft foods and liquids for the first few days after the procedure. Foods like soups, yogurt, mashed potatoes, and applesauce can prevent undue pressure on the treated tooth.
- Avoiding Hard and Sticky Foods: Hard or sticky foods can dislodge a temporary filling or crown and can also put undue pressure on the tooth before it’s fully healed. Foods like nuts, candy, and ice should be avoided until the final restoration is complete.
- Chewing on the Opposite Side: Until the crown is placed or the tooth is fully restored, try to chew food on the opposite side of your mouth.
Monitoring and Reporting
- Watch for Unusual Symptoms: While some discomfort and sensitivity are normal, severe pain, swelling, or an allergic reaction to medication should be reported to your dentist immediately.
- Regular Dental Visits: Even after the tooth has healed, regular dental visits are crucial for maintaining oral health and ensuring the longevity of your root canal treatment.
Conclusion
Recovery and aftercare following root canal therapy are vital to ensure a successful outcome. By managing discomfort, maintaining good oral hygiene, being mindful of your diet, and keeping regular dental appointments, you can promote healing and protect the integrity of the treated tooth.

